If patients receiving intensive care or undergoing major surgery develop excessively high or low blood pressures, they could suffer severe organ dysfunction. It’s not enough for their care team to know that pressure is abnormal. To choose the correct drug to treat the problem, doctors must know why blood pressure has changed. A new MIT study presents the mathematical framework needed to derive that crucial information accurately and in real time.
The mathematical approach, described in a recent study in IEEE Transactions on Biomedical Engineering, produces proportional estimates of the two critical factors underlying blood pressure changes: the heart’s rate of blood output (cardiac output) and the arterial system's resistance to that blood flow (systemic vascular resistance). By applying the new method to previously collected data from animal models, the researchers show that their estimates, derived from minimally invasive measures of peripheral arterial blood pressure, accurately matched estimates using additional information from an invasive flow probe placed on the aorta. Moreover, the estimates accurately tracked the changes induced in the animals by the various drugs physicians use to correct aberrant blood pressure.
“Estimates of resistance and cardiac output from our approach provide information that can readily be used to guide hemodynamic management decisions in real time,” the study authors wrote.
With further testing leading to regulatory approval, the authors said, the method would be applicable during heart surgeries, liver transplants, intensive care unit treatment and many other procedures affecting cardiovascular function or blood volume.
“Any patient who is having cardiac surgery could need this,” said study senior author Emery N. Brown, Edward Hood Taplin Professor of Medical Engineering and Computational Neuroscience in The Picower Institute for Learning and Memory, the Institute for Medical Engineering and Science and the Department of Brain and Cognitive Sciences at MIT. Brown is also an anesthesiologist at Massachusetts General Hospital and a professor of anesthesiology at Harvard Medical School. “So might any patient undergoing a more normal surgery but who might have a compromised cardiovascular system such as ischemic heart disease. You can’t have the blood pressure being all over the place.”
The study’s lead author is electrical engineering and computer science (EECS) graduate student Taylor Baum, who is co-supervised by Brown and Munther Dahleh, William A. Coolidge Professor in EECS.
Algorithmic advance
The idea that cardiac output and systemic resistance are the two key components of blood pressure comes from the two-element Windkessel model. The new study is not the first to use the model to estimate these components from blood pressure measurements, but previous attempts ran into a tradeoff between quick estimate updates and the accuracy of estimates; methods would either provide more erroneous estimates at every beat or more reliable estimates that are updated at minute time scales. Led by Baum, the MIT team overcame the tradeoff with a new approach of applying statistical and signal processing techniques such as “state-space” modeling.
"Our estimates, updated at every beat, are not just informed by the current beat; but they incorporate where things were in previous beats as well,” Baum said. “It’s that combination of past history and current observations that produces a more reliable estimate while still at a beat-by-beat time scale.”
Notably, the resulting estimates of cardiac output and systemic resistance are “proportional,” meaning that they are each inextricably linked in the math with another co-factor, rather than estimated on their own. But application of the new method to data collected in an older study from six animals showed that the proportional estimates from recordings using minimally invasive catheters provide comparable information for cardiovascular system management.
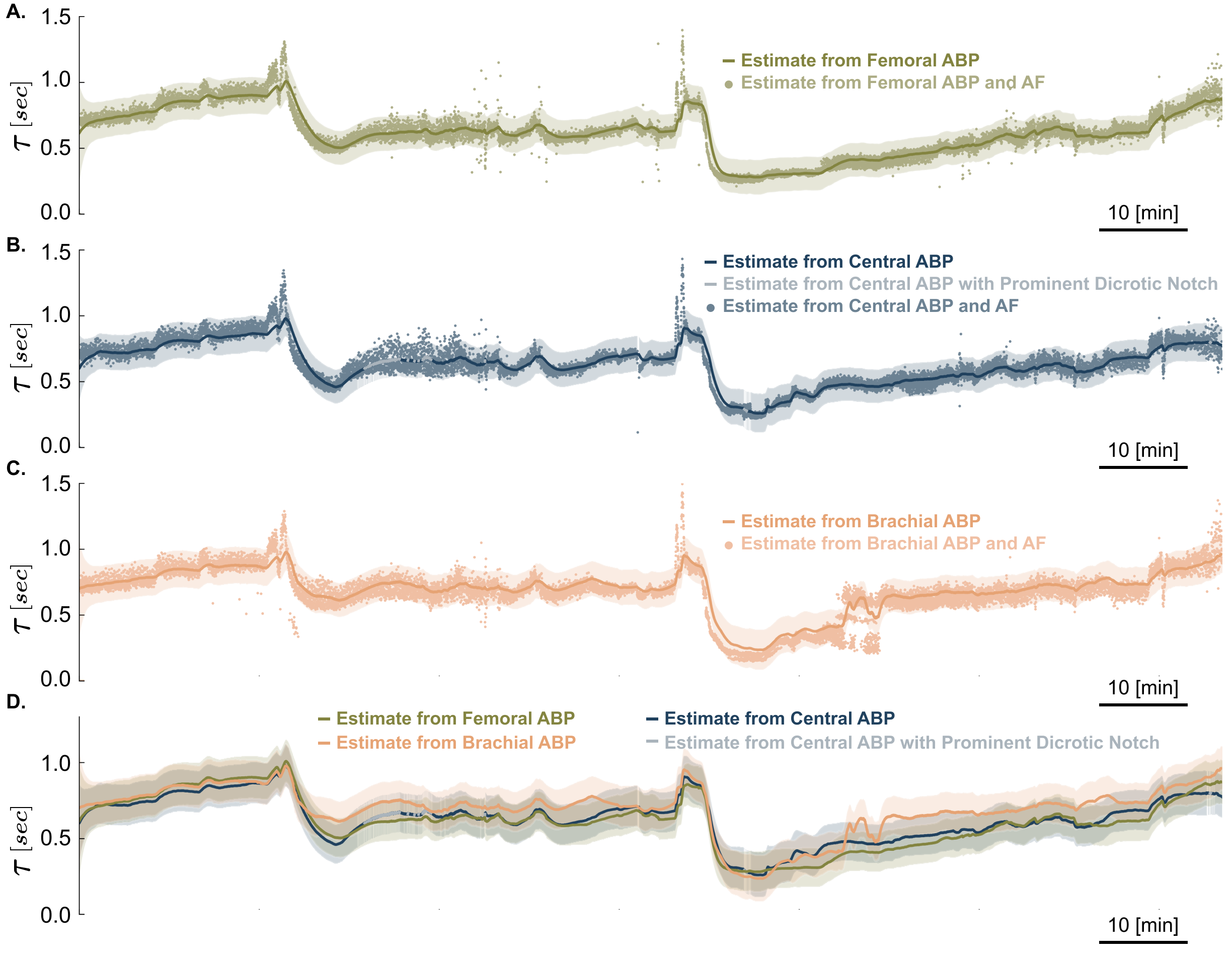
One key finding was that the proportional estimates made based on arterial blood pressure readings from catheters inserted in various locations away from the heart (e.g., the leg or the arm) mirrored estimates derived from more invasive catheters placed within the aorta. The significance of the finding is that a system using the new estimation method could in some cases rely on a minimally invasive catheter in various peripheral arteries, thereby avoiding the need for a riskier placement of a central artery catheter or a pulmonary artery catheter directly in the heart, the clinical gold standard for cardiovascular state estimation.
Another key finding was that when the animals received each of five drugs that doctors use to regulate either systemic vascular resistance or cardiac output, the proportional estimates tracked the resulting changes properly. The finding therefore suggests that the proportional estimates of each factor are accurately reflecting their physiological changes.
Toward the clinic
With these encouraging results, Baum and Brown said, the current method can be readily implemented in clinical settings to inform perioperative care teams about underlying causes of critical blood pressure changes. They are actively pursuing regulatory approval of use of this method in a clinical device.
Additionally, the researchers are pursuing more animal studies to validate an advanced blood pressure management approach that uses this method.
They have developed a closed-loop system, informed by this estimation framework, to precisely regulate blood pressure in an animal model. Upon completion of the animal studies, they will apply for regulatory clearance to test the system in humans.
In addition to Baum, Dahleh and Brown, the paper’s other authors are Elie Adam, Christian Guay, Gabriel Schamberg, Mohammadreza Kazemi and Thomas Heldt.
The National Science Foundation, the National Institutes of Health, a Mathworks Fellowship, The Picower Institute for Learning and Memory and The JPB Foundation supported the study.